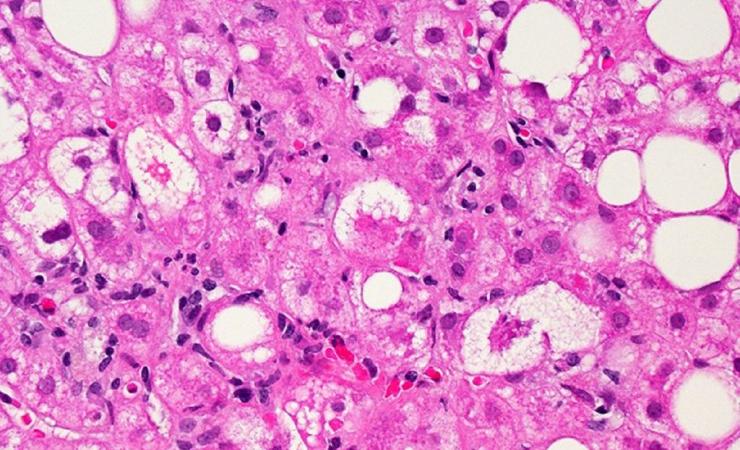
“It’s the most common disease you’ve never heard of,” says Prof. Quentin Anstee of Newcastle University, UK, referring to non-alcoholic fatty liver disease (NAFLD). In NAFLD, fat deposits build up on the liver – and in fact about a quarter of adults have this condition, particularly if they are overweight or diabetic, but it doesn’t bother them.
“For nine out of ten people, it really doesn’t matter too much. But about one in every ten people will get inflammation on their liver, and out of those ten people – so one out of 100 in total - one case will lead to scarring (fibrosis), cirrhosis and liver cancer,” says Anstee. This more severe version of NAFLD is referred to as non-alcoholic steatohepatitis, or NASH for short.
Currently, the only way to find out if you might be that one unlucky person in a hundred is to go through a liver biopsy – an invasive procedure which involves removing a small piece of liver tissue and examining it under a microscope.
The Innovative Medicines Initiative (IMI) project LITMUS project aims to revolutionise this testing process, so that patients can opt for a simple blood test or scan instead, which will reveal biomarkers that indicate earlier whether they will be the ones that have developed NASH or liver scarring so that the condition can be better managed.
Essentially, these innovations will both help to reduce the number of people who need to undergo invasive testing in routine clinical care, and also make recruitment into clinical trials more efficient so helping to develop better treatments. At present, up to 80% of people who undergo a liver biopsy to take part in a clinical trial are in fact unsuitable candidates, for example, not having NASH. The LITMUS strategy is to use a blood test or scan first, meaning that patients that do then go on to have a liver biopsy are more likely to be suitable for the trial, reducing the number of people who are unnecessarily biopsied.
“One of the big things is to make the case for the regulators that actually a blood test or a scan is as good at correlating to NASH and advanced fibrosis as a biopsy is. We've generated a lot of data showing that actually biomarkers can do the job just as well as biopsies, if not better, and can predict long-term outcomes,” says Anstee.
“It’s another part of changing the paradigm away from biopsies towards non-invasive testing for the clinical trials that are needed to get new medicines into the clinic.”
To make sure that the LITMUS methodology and process for finding and validating biomarkers was on track, the project submitted letters of intent to the US Food and Drug Administration (FDA) and the European Medicines Agency (EMA) addressing the use of these biomarkers to diagnose current disease severity and predict which patients will have worse long-term outcomes.
The successful interactions with the FDA and EMA indicate that the process used by LITMUS to assess biomarker performance are robust, and that essentially LITMUS can use these processes to submit the best performing biomarkers to the regulatory agencies, knowing that the data will be of the high quality required to support regulatory approval.
“This has really stress tested our processes and it’s a great step towards our goals for biomarker qualification,” says Anstee. “LITMUS has established a robust, technologically unbiased platform to assess biomarker performance at scale and pace. And we didn’t want to get to the end of the five years, take it to the regulators and have them say, you’ve got it wrong from day one.”
One of the key outputs of LITMUS is a large patient registry and biobank of blood and tissue samples from >10,000 patients that consists of data on patients with NAFLD. This major resource is the largest international database of the liver biopsy results of NAFLD patients who are currently undergoing follow-up. This will help support researchers to understand why some patients with NAFLD come to harm whilst others do not, and find better ways to diagnose and treat the disease.
Alongside independently assessing the performance of established biomarkers for use in clinical trials, LITMUS has also looked for new, even more accurate biomarkers – conducting major “multi-omics” studies that have helped identify several new biomarkers, that come from the liver, are correlated with liver scarring, and can be measured in the blood.
In early 2023, the project will lock the database for analysis and start to generate its final qualification packages to submit to the FDA and EMA. On the basis of these results, LITMUS will adapt its regulatory submissions to focus on the best performing tests and continue through the process.
As the project goes on, LITMUS will identify the most relevant biomarkers and work with them. Anstee says that the revolutionary, multi-dimensional dataset currently being compiled by LITMUS will lead to faster and better identification of these biomarkers, and the two letters of intent from the FDA mean that the project is well on the way to validating a series of biomarkers to identify those individuals who have the severe form of NASH so that medical care can be focused on the people that will benefit most.
LITMUS is supported by the Innovative Medicines Initiative, a partnership between the European Union and the European pharmaceutical industry.