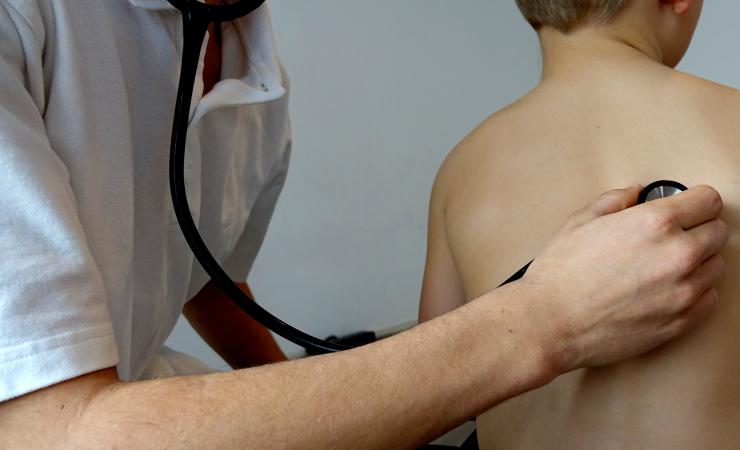
Despite extensive vaccination programmes, whooping cough (or pertussis) affected roughly 151 000 people in 2018, according to World Health Organization WHO) figures. The pertussis vaccines only protect people from developing serious illness, similar to their COVID-19 counterparts.
Recent research supported by the Innovative Medicines Initiative (IMI) through the PERISCOPE project shows that older children tend to have more nasal antibodies against the whooping cough bacteria than younger children, most likely because they have been exposed to it more often. The older children’s immune response is further improved after a booster vaccination against the pathogen. The research, published in Nature Communications, can help immunologists to better understand how infections can shape people’s immune memory.
Although vaccinations have kept pertussis under control in Europe, the disease still circulates throughout Europe and beyond, causing severe infections in those without the full course of vaccines. The paper’s authors wanted to see how this circulation affected people’s immune response.
“There is a huge under-diagnosis of pertussis, either because pertussis infections are milder in vaccinated individuals, because people are simply not thinking of pertussis, or because a diagnostic test is not done until it’s too late to detect pertussis,” said Dr Dimitri A. Diavatopoulos of the Radboud Center for Infectious Diseases in Nijmegen, The Netherlands.
Since there is no truly specific immune biomarker for pertussis infections, the researchers wanted to find a way to determine whether a person’s pertussis immunity is from the common pertussis vaccine or from exposure to the pathogen.
They first studied two age groups, one between 7-10 years old and the other 11-15 years old. Both groups had received their full pertussis shots from the Netherlands’ national vaccination programme. They received the common acellular pertussis vaccine, which uses the disease-causing Bortadella pertussis bacteria’s antigens rather than the whole bacteria.
Both groups were then given booster shots and the researchers tested for pertussis antibodies by using absorbent strips to collect fluid from their noses (the common entry point for pertussis infections). The researchers did these swabs three times: on the day of the booster, after 28 days, and then one year after the booster.
The nose swabs showed that the older group had more vaccine antibodies after their vaccination than the younger group. Although the amount of antibodies declined in both groups after the booster, the decline was much slower in the older group. This, explains Dr Diavatopoulos, is likely due to previous exposure to the pathogen causing more durable antibodies in the older children.
“The difference in waning of vaccine-induced antibodies was definitely not something that we expected when we started the study,” he said. “This tells us is that immunity is not static, and continues to evolve as we grow older and experience infections as well as booster vaccinations.”
Dr Diavatopoulos and the other researchers now hope to follow up on this early research with a larger, international sample size. He and the paper’s co-authors want to continue finding out how vaccines lead to durable protective immunity for both individuals and wider society, and the role that exposure to pathogens plays in this process.
“This question is not only relevant for pertussis, but also for other pathogens that continue to circulate, including coronavirus,” says Dr Diavatopoulos.
PERISCOPE is supported by the Innovative Medicines Initiative, a partnership between the European Union and the European pharmaceutical industry.